ECMO explained: The specialist life support key to our Covid-19 response
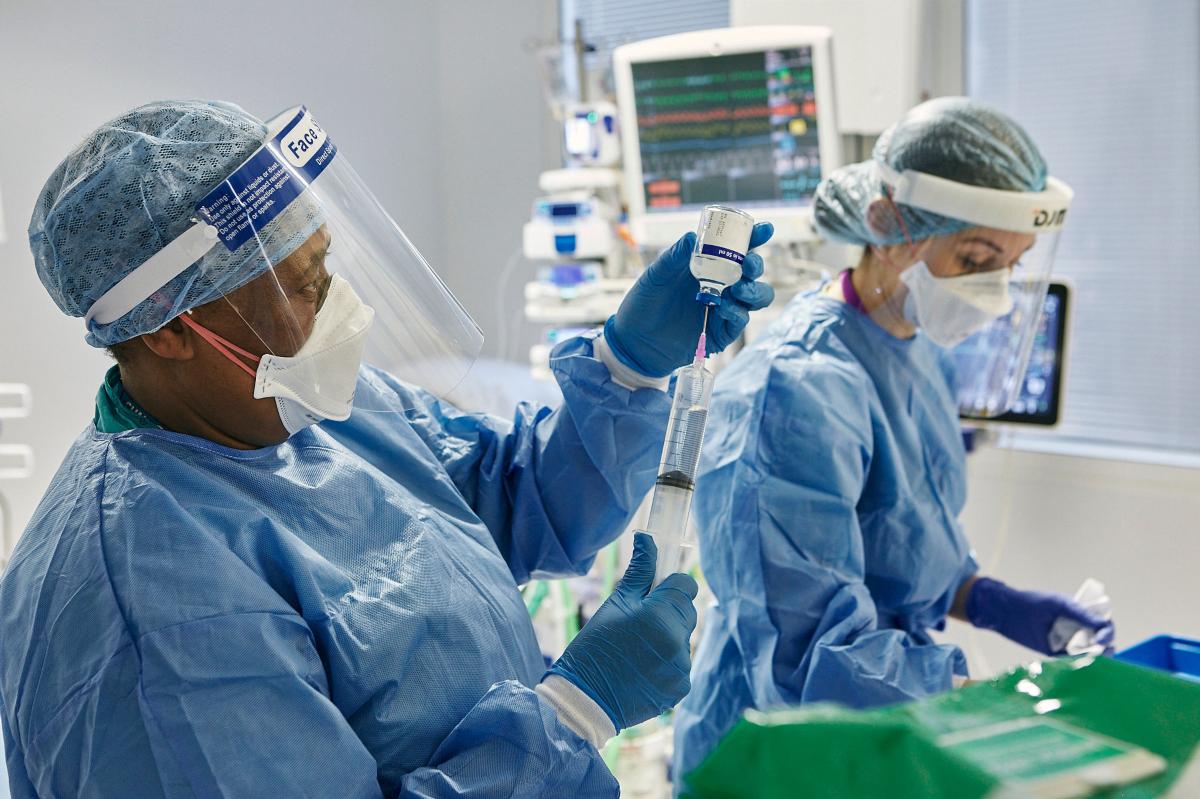
The sharp rise in hospital admissions during the first coronavirus peak included a number of people suffering from respiratory failure.
Unable to breathe for themselves, even with the help of a ventilator, these patients urgently required specialist support in the form of an ingenious machine that temporarily replaces the function of the heart and lungs.
Extracorporeal membrane oxygenation, or ECMO for short, transports blood from the body to an artificial lung (oxygenator) that, like the human lungs, adds oxygen and removes carbon dioxide.
The machine then returns the blood to the body via a pump, with the same force as the patient’s own heart.
Whilst some patients can be on ECMO for just a few hours, it typically supports more seriously ill patients for up to two weeks, whilst their organs recover and can operate unaided.
The ECMO service at Barts Health was established in 2016 and forms part of Barts Heart Centre – the largest specialist cardiac centre of its kind in Europe. The team see between 40 and 50 ECMO patients in a normal year and treat around one to two patients at any one time.
Between April and June 2020, as the pandemic took hold in the UK, they acted as a ‘surge centre’ for cases in and around the capital, receiving 18 patients with coronavirus – approximately ten per cent of all Covid-19 related ECMO cases across the UK.
At the peak in mid-April, they were caring for 11 people simultaneously, including a number of healthcare workers who were critically ill.
 Dr Sachin Shah, ECMO director and intensive care consultant, said: “The enormous scaling up of the service, and in such a short space of time, was possible because of the dedication and experience of the team.
Dr Sachin Shah, ECMO director and intensive care consultant, said: “The enormous scaling up of the service, and in such a short space of time, was possible because of the dedication and experience of the team.
“Everyone came together at a crucial moment.”
The specialist staff and equipment required to provide ECMO safely means it’s only available in a small number of UK hospitals.
Alongside intensive care doctors and nurses, it also involves a large multidisciplinary team of healthcare assistants, perfusionists, pharmacists, physios, dieticians, speech therapists, and many other support services.
Barts Health provides a 24/7 service, meaning patients can start on ECMO therapy at a referring hospital, before being transported to St Bartholomew’s Hospital to continue their treatment.
Dr Shah said: “We have well-defined pathways, from referral to discharge, encompassing end of life care, psychosocial support and even follow-up appointments for those we successfully send home.”
Patient outcomes before the pandemic were very good, with both survival and complication rates, and patient satisfaction, comparing favourably with other units both in the UK and internationally.
The team’s hard work was recognised in April when dealing with a sharp rise in coronavirus cases locally.
78% of Covid-19 patients treated with ECMO at St Bartholomew’s Hospital survived and were discharged.
A recent peer review also praised the service for its responsiveness, quality of advice and collaborative approach.
Dr Edward Rowland, medical director at St Bartholomew’s Hospital, has commended the team for their key role in pandemic to date.
“The quality of care delivered by the ECMO service is state-of-the-art and, in so many ways, an example to all the other units in the country.
“It should be a source of immense pride that amongst this outstanding practice is the holistic care for patients and families, both for survivors and those at end of life.”
“Without this machine I don't think I would be with my children now"
Mandy Nguyen was fighting for her life after falling ill with Covid-19 at 32 weeks pregnant.
Three weeks earlier, on 6 April 2020, Ms Nguyen had given birth to her son Wyatt through an emergency caesarean section at The Royal London Hospital.
He was two months premature but was healthy. However, Ms Nguyen took a turn for the worse.
Doctors had told her family to prepare for the worst, because coronavirus had ravaged her lungs to the point she could no longer properly oxygenate her blood.
She was taken to St Bartholomew's Hospital, where she was attached to an ECMO machine.
The machine temporarily replaces the function of the heart and lungs. It is only used on patients unable to breathe for themselves, even with the help of a ventilator.
After three weeks on ECMO Mandy woke up.
“I felt lucky to be on this machine.
"I'm ever so grateful, as without this machine I don't think I would be with my children now," Mandy said.
The experience has left her "extremely grateful for the NHS".
"I just want to say thank you. People don't see this side of the NHS, the little things they do for you," she said.
Read the full story on the BBC News website.
Pictures courtesy of Matthew Andrews
Read more
