Wearing a mask is no different to wearing your seatbelt
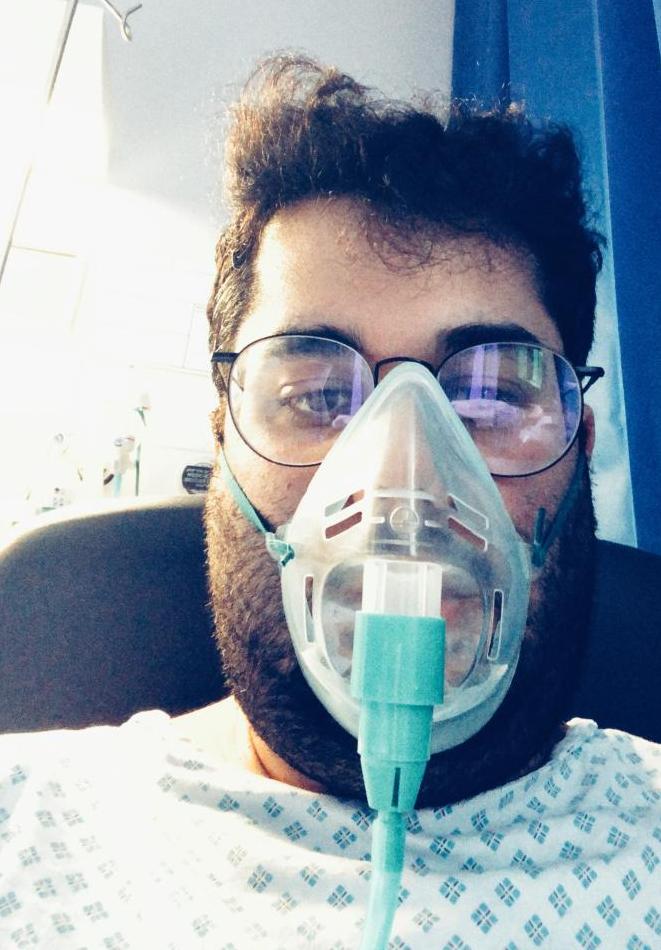
Shimol Khakhar speaks out about his 20-day experience in ITU at Newham Hospital after contracting coronavirus, praising staff and urging others to listen to advice and take the illness seriously.
The 30-year-old movie buff describes how staff saved his life and gave him hope during his challenging period of illness.
It all started around a week before lockdown was announced, in mid March. At this point I was already working from home but I was starting to feel achey and feverish. Although I have type 1 diabetes, I am otherwise a healthy young person so I was sure it would just be a regular fever and not Covid-19. Nonetheless, I began self-isolating immediately as soon as I noticed symptoms.
It soon became clear that what I had was not a regular fever as my symptoms became progressively worse. While my symptoms were initially manageable, within a few days I had a full blown fever and by day 5, I had shortness of breath and was coughing continuously.
By this point I did not feel in control of my fever or my rational thinking. Being diabetic, this was a big problem because I was not able to control by insulin or manage my condition by eating food on time. I held out until Day 7, which I understand is when symptoms are supposed to clear.
However, my symptoms didn’t subside so I called NHS 111.
As you may understand I was unlucky enough to fall ill at the very beginning of the pandemic when our healthcare services were still trying to understand the virus and put measures in place to care for the masses. However, this did mean that when the paramedics came, they didn’t believe I was sick enough to go to hospital and advised me to stay at home and call back if I didn’t start to recover.
Unfortunately, I wasn’t showing any signs of recovery. After three further days my symptoms became completely unmanageable; my fever worsened and I had headaches, coughs, nausea and extreme difficulty breathing. In fact, my housemate kept coming to check on me because I was struggling breath. She was worried I would stop breathing completely. I called my parents who were shocked to see the state I was in and who immediately called an ambulance.
When the paramedics arrived they gave me oxygen and it honestly felt like new life was being breathed into me. I want to also stress how wonderful these paramedics actually were. Initially when they arrived I felt a slight tinge of shame. After over a week of being unwell I wasn’t really able to have regular showers or get dressed and my room wasn’t looking particularly great since I’d been holed up in it. Nonetheless, the paramedics treated me with nothing but dignity and respect and their kind faces were exactly what I needed. I was taken to Newham Hospital and admitted to ICU.
To be totally honest, I don’t remember a great deal from this period. However, one of the first faces that really stuck out to me was that of my doctor - Dr Neera Patel. The care and patience she took in explaining every small detail of what they were going to do to treat me made such a huge difference. While I don’t know exactly how many people in the hospital had been admitted with coronavirus, I could tell I was one of many patients staff were frantically doing their best to keep alive. Nonetheless, Dr Neera addressed me by name and treated me like a human. She even spoke to my parents over the phone to reassure them and explain any treatment I was having.
I do however want to stress, for anyone who has been hospitalised, even with the best staff in the world it can be a very lonely and isolating time. Because staff had to wait for a Covid-19 positive test result, I was moved to a private room, while waiting for my swab results. I rarely saw anyone aside from the staff who would pop in to check on me. Not being able to see my family or my wonderful partner of three years on top of being incredibly sick meant my mood was the lowest it had ever been.
At one point I asked Dr Neera if I was going to die and she said:
“Not on my watch. You’re the same age as me, you can survive this. Just lie down, disconnect from social media, watch ‘Friends’ on TV and focus on breathing. We will take care of you.”
After nine days in ICU, I finally heard the words I’d been waiting for: “You’ve made good progress and you’re on the road to recovery, we can discharge you!” I finally returned home to my flat and under strict orders from Dr Neera I avoided social media and concentrated on getting better. Although the worst was over I was facing months of recovery at home to fix the damage Coronavirus had done.
At this point I was definitely feeling much better but my oxygen saturation levels were still pretty low. This meant that performing even the most basic of tasks was a huge effort. Luckily for me I had the support of a local community group in my area, the Waterside Park Community Champions, my incredible partner, and my parents. Without them I would have really struggled. Although I’ve lived in my flat for seven years I’ve never spoken to many of my neighbours. However, these same people took the time and effort to cook home made meals and leave them outside my door everyday. I will be forever grateful to them.
However, my journey to recovery, like many others who have had coronavirus, was a complicated one. A week after I had been discharged I was still coughing and developed a severe pain in my chest over the easter weekend. I thought I had broken a rib and rang my GP for advice. They advised me to ring a paramedic who was with me in around 20 minutes. It turned out I had complex phneumothorax, in other words a collapsed lung. So back I went to Newham Hospital, this time isolated from the other patients as I was one of the few on Heather Ward who didn’t have coronavirus! I was treated with high flow oxygen to reinflate my lung. There was not much else I could do but be patient and wait for my body to recover. However, there were two stand out moments which I’d like to bring attention to.
At this point I’d had pretty much the same thing for breakfast, lunch and dinner. Being lactose intolerant, there wasn’t always much choice and occasionally I missed having a full meal. Dr Neera heard I was struggling with this and went out of her way to bring me a meat biriani which she had received as part of a donation to NHS staff. It was honestly the most amazing thing. I could have cried!
There was also one nurse I would regularly banter with about my food, my breakfast often having to plain toast because of my dietary needs. We spoke about our love of full English breakfasts. On my last night, I was woken up at around 5am by this kind nurse who had brought me sausages, bacon and hash browns hot from the canteen. This time I did cry.
On 18 April, I was discharged. Since then I have applied for as many Covid-19 clinical trials as I’m eligible for and am currently involved in two antibody test trials being run at Barts Health. Having been through coronavirus, I will do anything I can to prevent others having to go through the same thing. Something good has to come from what I went through, I have to try to help fight this any way I can.
 [Image: Shimol and his girlfriend before the pandemic]
[Image: Shimol and his girlfriend before the pandemic]
While I had incredible care from the staff that looked after me, support from my local community, and my fantastic partner and parents, I want to stress the effect Covid-19 has had on both my mental and physical health. I still have post traumatic stress disorder from my ordeal and life long issues with my lung capacity. With lockdown easing I’m worried people may start to relax on important safety requirements such as social distancing and wearing a mask. To these people, I say:
Wearing a mask is no different to wearing a seatbelt. Practicing social distancing is no different to standing back from the platform edge. Please do your bit to stop the spread of Covid-19.
Anyone can get coronavirus and there’s no guarantee around how your body will cope with the it.
