What's it like working in one of the most war-torn countries?
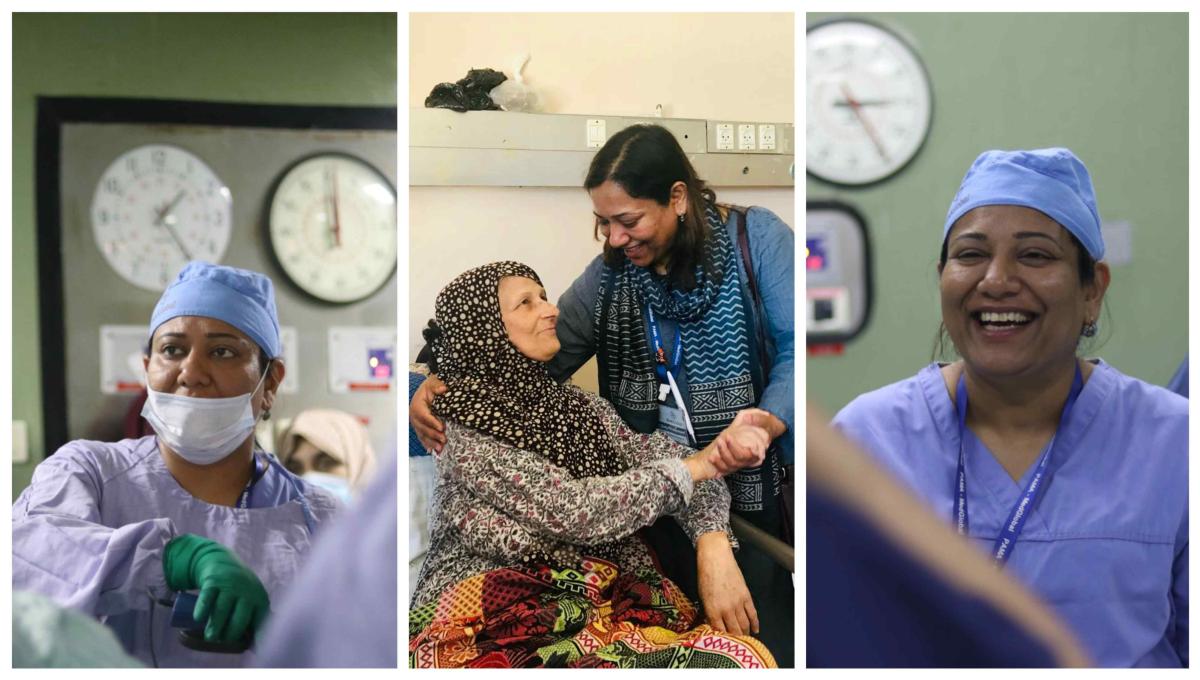
Arti Garg, Surgical Consultant at Newham Hospital, has just returned from a 8-day trip to Gaza, where she provided much needed surgical support to patients and shared her expertise with healthcare staff. Here, she describes her experience.
Can you remind us of the purpose of your trip and what you did in Gaza?
With the support of the MedGlobal charity, the Palestinian American Medical Association (PAMA) and Ministry of Health Gaza, myself and a team of medical surgical volunteers from around the world travelled to Gaza to help support Al-Shifa, Nasser and Rantisi Hospitals providing medical consultations, performing surgical procedures and offering medical training to local healthcare staff. I would also like to highlight that while the country is facing a crisis – I was greeted like an old friend when I arrived and couldn’t praise the hospitality of my colleagues who work there more. The people of Gaza, patients and staff were all incredibly kind.
My expertise is in performing surgery on general surgical and colorectal cases, so much of my time in Gaza was spent performing laparoscopic procedures and colectomies on patients suffering from cancer and other chronic bowel conditions. I also provided training and guidance in these areas to other doctors in the Al-Shifa hospital .
What kind of health challenges is the country’s healthcare system facing?
The country is facing a myriad of healthcare challenges, the first of which being that it is massively impeded by a shortage of medical supplies and medications. Nearly 1.6 million people in Gaza are in need of humanitarian assistance and last year almost 50% of essential medications were at zero stock level. Due to restrictions on leaving the country access to healthcare specialists are limited. There were no paediatric surgeons, radiation oncologists, mental health support staff, or screening specialists.
One of the biggest challenges I faced was the lack of laparoscopic disposable instruments and equipment. An equally difficult challenge was coming to terms with sometimes having to operate in the dark. While myself and my surgical colleagues were performing long operations the electricity would fail around 4-5 times and we would be left without power, mid-surgery for around 60 seconds before the back-up generator kicked in.
The utter resilience and exceptional willingness to provide the best care possible despite the circumstances is a real credit to the healthcare staff who work there. They are truly wonderful.
What kind of surgical expertise did you offer the Gaza team?
In the UK there is one doctor for every 300 people. In Gaza there is one doctor for every 1,500 people. Thus it was extremely important that we imparted as much knowledge as possible so the doctors are armed with as much expertise as possible to care for patients in a pressured environment. Indeed, many of the complex and intricate operations simply wouldn’t have taken place if not for the experience and skills our volunteering team were able to bring to the operating table.
Some of these included particularly complex operations such as a laparoscopic anterior resection with total mesorectal excision. This is where the left side of colon and part of rectum is removed along with blood vessels and lymph nodes and re-joined to another part of the intestine, separating the cancerous tissue and preventing it from spreading.
I was also very pleased to have had the opportunity to deliver a key note at the Colorectal and Liver Metastases Symposium . Almost all of the surgical and allied speciality faculty from Gaza attended.
What key learnings have you brought back with you?
Working in a country where resources are extremely limited got me thinking about the importance of a sustainable healthcare system. Due to stock shortages in the Gaza hospitals nothing was ever really disposable. Instruments would be cleaned and re-used as many times as possible so that more patients could be treated and cared for. We are very lucky to live in a country where we are in a position to use disposable operative instruments and have a multidisciplinary care model in the best interests of patients.
However, I do believe that to achieve a healthcare system that works well, we need to look at how we can become more efficient; perhaps by considering using instruments which are not disposable yet still maintain patient safety. I also witnessed first-hand the impact that appropriate training and effective transferring of skills can have on a system in terms of making it more independent and ergonomic.
I am now working on a project to assess the role of futuristic technologies such as clinical artificial intelligence’ in resource poor settings to optimise the healthcare matrices of the region.
How can others get involved?
This experience has been one-of-a-kind and I intend to work with the MedGlobal charity on offering this kind of support again very soon, as it is an ongoing mission. I would encourage all doctors who have the capacity to get involved. You can do this by emailing MedGlobal.
Alternatively you can visit the MedGlobal charity website for more information.
I would also like to take this opportunity to thank the management team at Newham Hospital and Barts Health NHS Trust who encouraged and supported me to pursue this journey. Their help and support has been invaluable in enabling me to partake in this expedition.
How would you describe your experience in three words?
Unique, eye-opening, fulfilling…
Arti Garg
Surgical Consultant
